Insurance claims have always been the most critical moment of truth between insurers and customers. When a policyholder files a claim, the speed and accuracy of the response often determine trust in the insurer. Yet traditional claims management processes are slow, paperwork-heavy, and prone to manual errors. According to a report by McKinsey, insurers that adopt automation in claims operations can improve the accuracy of routing claims to the appropriate teams by 30 percent.
For insurance executives, the question is no longer whether automation is needed, but how to implement it effectively. Automated claims processing is transforming the way insurers evaluate, approve, and settle claims by replacing manual workflows with intelligent digital systems. In this guide, we will explore what automated claims processing is, how it works, the technologies behind it, its key benefits, and the practical steps insurers can take to successfully implement claims automation.
What is Automated Claims Processing
Automated claims processing allows insurance companies to use digital technology, artificial intelligence, and workflow automation to manage claims from submission to settlement, with little to no human involvement.
In a manual, claims processing agents must confirm documents one at a time, confirm policy coverage, evaluate claim eligibility, and approve payments. This is a time-consuming process and increases costs to the company. An automated claims processing software replaces manual documents with data-driven intelligent workflows, policy rule validation, fraud detection, and automated claim payouts.
Automated claims processing technology allows insurance companies to process large volumes of claims while maintaining accuracy and compliance. Automation has also been embraced in the processing of other types of claims in insurance, such as health, motor, property and casualty, travel, and life insurance claims.
Automated claims management allows insurance companies to integrate claim submission, validation, evaluation, and payment automation in one digital system.
How Automated Claims Processing Works
An automated insurance claims processing workflow integrates multiple technologies to process claims faster and more accurately. While implementations vary, the general workflow follows a structured sequence.
1. Claim Submission
Policyholders can submit claims through the mobile app, website, and email. The automated claims software captures and processes data, documents, and supporting items, including pictures, receipts, and medical records.
2. Data Extraction
Manual data entry can be eliminated, along with a reduction of associated errors, through the use of Optical Character Recognition and Gen AI data capture tools.
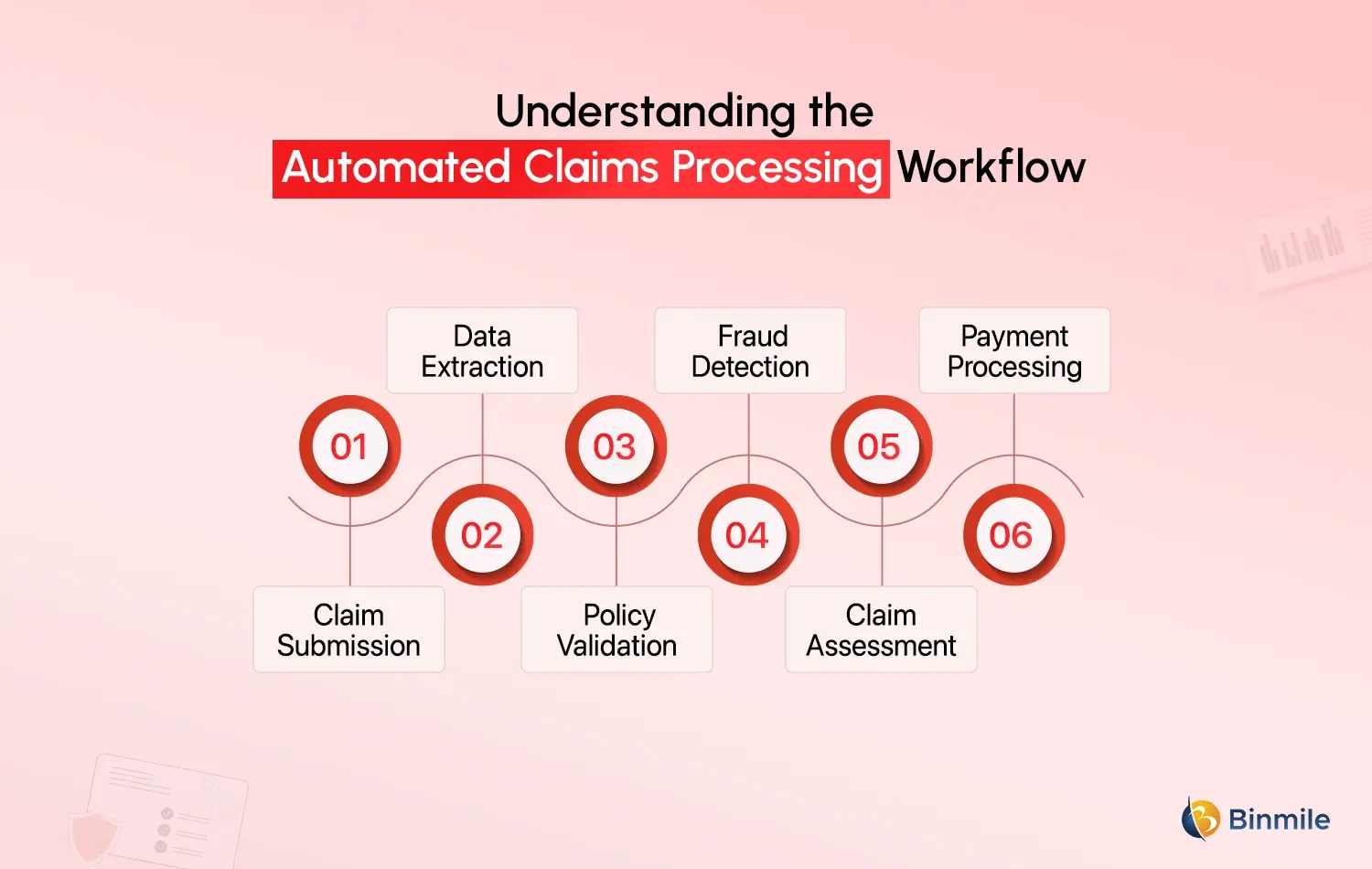
3. Policy Validation
Automated claims processing systems can verify terms of the policy, including coverage amounts, exclusions, and conditions of eligibility, using policy databases.
4. Fraud Detection
Artificial Intelligence claims processing and analyzes data patterns, previous claims, and behavioral data to detect fraudulent claims.
5. Claim Assessment
AI in insurance and rule-based engines determine the eligibility of a claim based on policy criteria and history. Simple claims may be flagged and receive automatic approval.
6. Payment Processing
Automated claims systems trigger payments through associated financial systems. Clients receive updates through email, text, or app notifications.
What are the Core Technologies Behind Automated Claims Processing
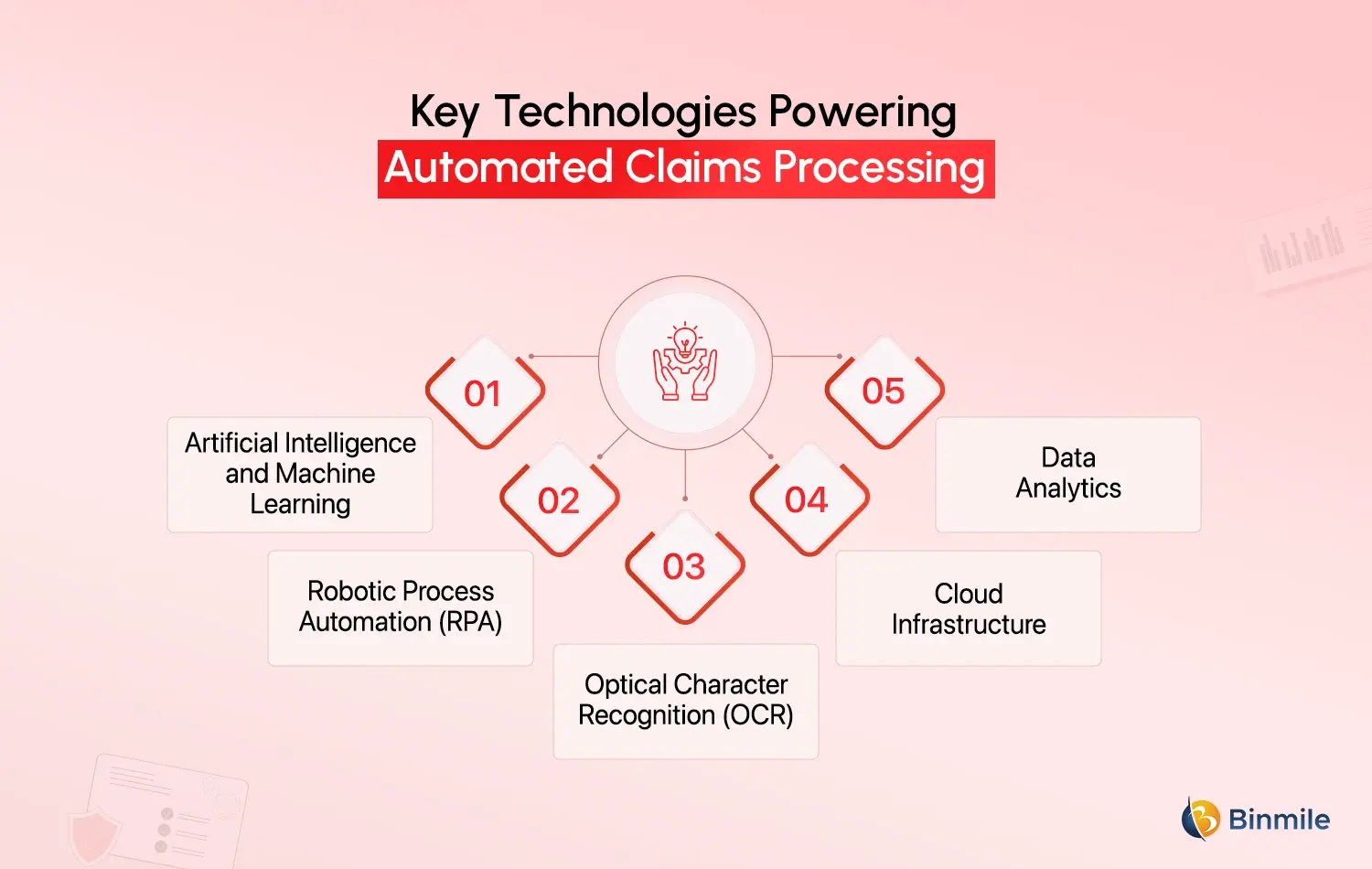
Several advanced technologies power modern automated claims processing systems. Together, they create a digital ecosystem capable of managing complex claims operations.
-
Artificial Intelligence and Machine Learning
AI models assess claims data to identify case fraud and determine the status of claims. Additionally, AI claims processing allows for automated damage assessments through the use of image recognition.
-
Robotic Process Automation (RPA)
Bots of RPA systems take over basic, monotonous duties, including data entry, verification of claims, transferring of documents, and initiating payments. As a result, this tool is applied in almost every claims automation project.
-
Optical Character Recognition (OCR)
OCR speeds up document processing, as it is able to pull out text and data from documents and form claims, scans of invoices, and medical reports.
-
Cloud Infrastructure
Cloud services offer the flexibility to manage hundreds of claims concurrently, while also providing them with the up-time requirements.
-
Data Analytics
Data analytics help in improving decision-making by assisting insurers in analyzing the patterns of the claims. It also assists in finding operational inefficiencies as well as in assessing the claims.
Explore scalable automated claims processing systems designed for modern insurers.
What are the Key Benefits of Automated Claims Processing
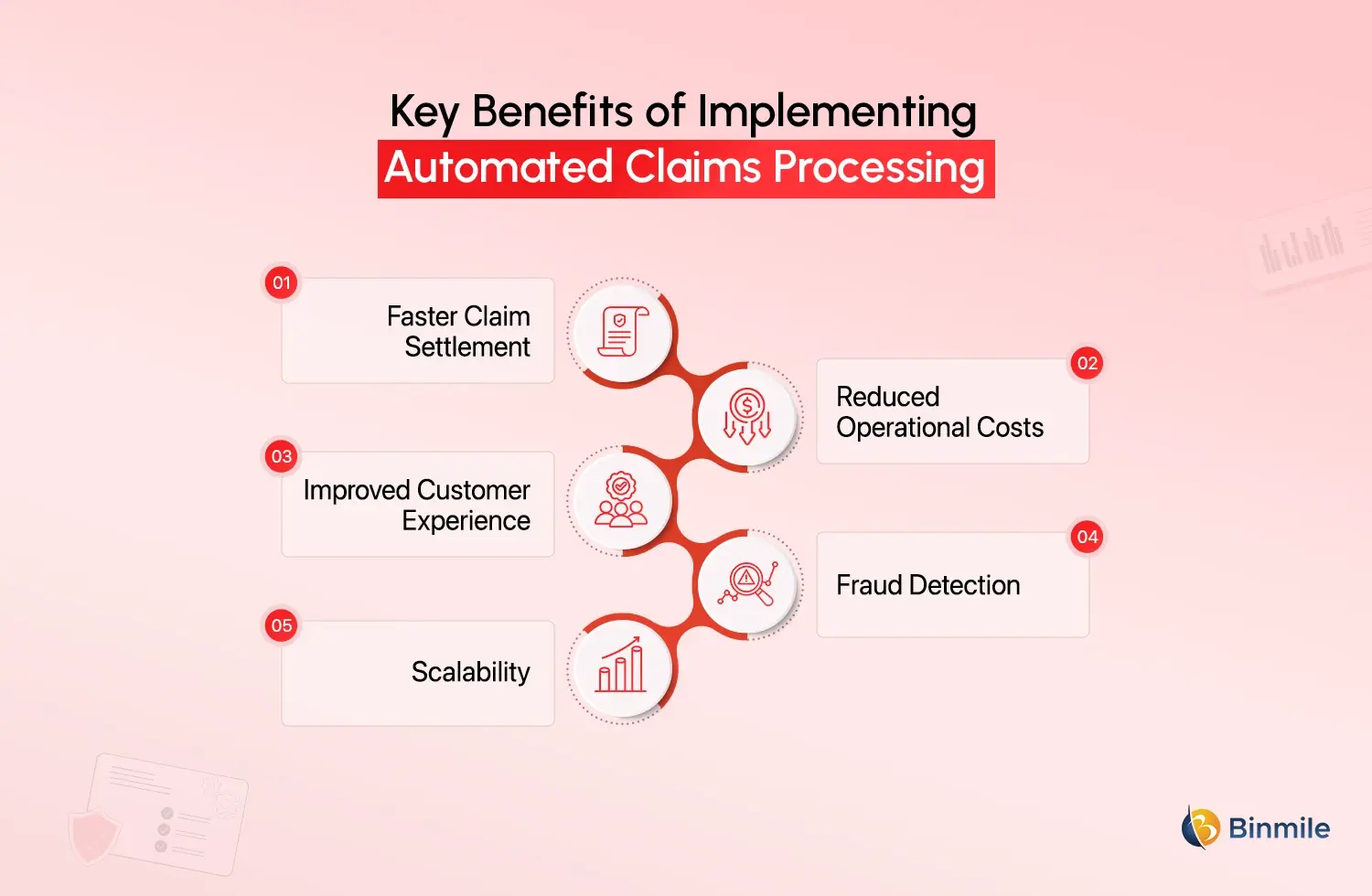
The benefit of automated claims processing goes far beyond operational efficiency. Furthermore, it directly impacts customer satisfaction, cost management, and competitive positioning.
-
Faster Claim Settlement
Automation speeds up claim processing and cuts processing times from days to hours. Additionally, Straight-through processing technology can approve claims instantly.
-
Reduced Operational Costs
With automation, fewer people are required to work in the claims department, decreasing the amount of manual labor required and decreasing the amount of paperwork created.
-
Improved Customer Experience
With automation, customers are able to track the status of their claims and receive payout notifications and claim status updates. All of this increases retention and the trust policyholders have in the business.
-
Fraud Detection
With automation, businesses are able to detect fraudulent claims and other suspicious activities that may go unnoticed when the claims processing is done manually.
-
Scalability
With automation, businesses are able to handle claiming spikes. When there is a natural disaster, businesses can handle the increased amount of claims.
Key Components of an Automated Claims Processing System
A successful automated claims processing system typically includes several integrated components.
| Component | Role in Claims Automation | Claim Intake Portal | Enables digital claim submission through mobile or web interfaces |
|---|---|
| Document Processing Engine | Extracts and validates information from claim documents |
| Policy Verification System | Confirms policy coverage and eligibility conditions |
| Fraud Detection Engine | Identifies suspicious claims using AI analytics |
| Workflow Automation Engine | Manages claim routing, approvals, and escalation processes |
| Payment Processing Integration | Initiates settlement payments automatically |
How to Automate Insurance Claims Processing
Implementing insurance claim automation processing requires a structured approach that combines technology adoption with operational improvements. To begin, insurers should investigate and assess existing claims workflows in order to pinpoint delays, areas of inefficiency, and repetitive manual tasks that can be automated.
The following step involves configuring claim submission to be done online or via a mobile application, digitizing claim submission, and allowing customers to submit claims and required documents electronically. This both eliminates the need for paper records and guarantees order within the submission. Robotic process automation and other similar workflow automation technologies can be utilized to perform tasks such as document checks, policy analysis, and case routing.
The use of Artificial Intelligence (AI) in decision making process is also recommended for routing the complex claims to human analysts and for directing the simple, straightforward, and already approved claims to the AI. This also improves the decision-making process of the claims being analyzed. The implementation of the automation framework to operational fundamentals such as policy processing, billing, and customer service is also recommended for improving data flow.
Fraud, automation frameworks, and other systems can also be improved through continuous analysis for the refinement of the system and improved performance within the system. This, in turn, also allows for the improvement of digitally automated claims systems. Additionally, improved claims processing systems are the product of enhanced analyses. In the end, the improvement of the automated Digital claims systems can also be achieved through leveraging technologies and operational revisions.
Challenges in Automating Claims Processing and How to Overcome Them
Despite its advantages, implementing automated claims processing systems can present several challenges.
-
Legacy System Integration
Many insurers run on outdated core systems that make integrations with newer automation technologies next to impossible.
Solution
Implementation of API based middle-ware and microservices to automation frameworks.

-
Data Quality Issues
Automation is reliant on accurate data that is adequately structured. Poor data quality is an automation efficiency limitation.
Solution
Data governance and AI data validation.
-
Regulatory Compliance
Insurance policies need documentation, transparency, and audit trails.
Solution
Build automated workflows around compliance and capture every claim decision.
-
Employee Resistance
Concerns around automation replacing employee jobs are common.
Solution
Help employees see automation as a productivity feature that enables adjusters to concentrate on intricate claims and remove the mundane.
Discover how automated claims processing solutions can streamline workflows, reduce costs, and improve customer satisfaction.
How Technology Partners Can Accelerate Claims Automation
Automating insurance claims is complex, requiring expertise in Artificial Intelligence, workflow automation, system engineering, and legal and regulatory constraints. Insurers have a hard time shaping these efforts, especially when trying to keep business as usual.
However, InsureTech app development and business process automation, as well as custom software development companies, have the expertise to modernize claims infrastructure for insurers without impacting business operations.
When Robotic Process Automation, real-time analytics, and artificial intelligence are combined with process automation, claims processing is radically improved. Custom insurance software development companies, automation, and insurance software development with process automation can provide insurers with custom solutions for their unique processes.
Companies like Binmile help insurers modernize their infrastructure and automation to enhance their claims processing systems, ensuring high claim traffic while remaining compliant with industry regulations. Additionally, with insurance app development automation, AI claims workflow, and integrated enterprise systems, insurers can enhance their operational efficiency and improve customer satisfaction.
Frequently Asked Questions
Many routine and structured claims can be automated, including health insurance reimbursements, motor damage claims, travel insurance claims, and simple property claims. Complex or high-value cases are typically routed to human adjusters for detailed evaluation.
Successful automation requires a clear strategy, strong data management practices, employee training, and integration with existing systems. Starting with pilot projects and gradually expanding automation helps insurers minimize operational disruptions.
Automation eliminates repetitive manual tasks such as document verification, policy validation, and data entry. This reduces staffing costs, improves efficiency, minimizes errors, and accelerates claim settlements, leading to significant operational savings.
Yes, modern automated claims processing systems are designed with strong security frameworks, encryption protocols, and compliance mechanisms. They maintain audit trails, follow regulatory guidelines, and protect sensitive policyholder data.
No. Automation handles repetitive and rule-based tasks, while complex cases still require expert judgment. Claims adjusters focus on investigations, negotiations, and unique situations where human decision-making is essential.
Automation is most effective for high-volume claims such as health, motor, and travel insurance. However, with advanced AI capabilities, automation is gradually expanding into more complex insurance segments.
Core technologies include artificial intelligence, machine learning, robotic process automation, optical character recognition, cloud infrastructure, and advanced analytics. Together, they enable intelligent decision-making and efficient workflow automation.
Executives should evaluate system integration requirements, data readiness, regulatory compliance, scalability, and long-term operational benefits. Choosing the right technology partner is also critical for successful implementation.









